Villainous blood clots: Is the fear justified?
It’s been over a year since the emergence of the COVID-19 pandemic and with an increasing number of vaccinated people, fears of newly developed vaccines are also on the rise. The media is filled with information about the connection between certain vaccines and blood clots but is this fear really justified? Before you refuse the jab, it is important to understand what blood clots are, how common they are, and what is their connection with COVID-19 and the vaccines.
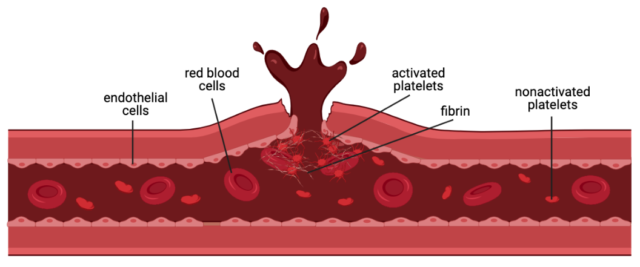
Blood clots are an important part of our immune system preventing us from bleeding out from minor injuries and surgeries, thus saving our lives. Under normal conditions, platelets (thrombocytes) circulate in the bloodstream in a deactivated state. When they notice a bleeding vessel wall (endothelium), they immediately rush towards the site of injury to repair the damage, attaching to said site by special receptors and get activated. This activation changes their function and structure from disc-shaped to spherical with cellular extensions called filopodia resulting in platelet aggregation. Moreover, soluble fibrinogen changes into insoluble fibrous fibrin holding the clot together and making it more stable 1. Once the blood vessel is fully healed, a blood clot known as a thrombus naturally dissolves.
Problems may arise for several different reasons. For example, blood clots might begin forming on their own without a preceding injury. Other times, due to various underlying health conditions, these blood clots do not dissolve but remain attached to the blood vessel. If the thrombus is large enough, it might block the blood flow, preventing the transportation of blood to tissues or organs and depriving them of oxygen, leading to damage or even tissue death. The situation gets even more dangerous when blood clots detach and travel through the circulatory system to the brain, heart, or lungs where they can subsequently cause a heart attack, stroke, or lung embolism. This might sound scary, but there are many drugs like thrombolytics, which dissolve blood clots, and anticoagulants (also known as blood thinners) that prevent blood clot formation 2.
Some people are more susceptible to excessive blood clotting, or coagulation. This can be the result of several risk factors, like genetic predisposition, age, obesity, bad diet, and lack of movement (even long travelling by car or plane). Different therapeutics such as nonsteroidal anti-inflammatory drugs (NSAIDs) like aspirin, some antibiotics, or estrogen in contraceptives can also contribute to blood clot formation. Women are, in general, more prone to blood clot formation because of contraceptive use and childbirth, where there is significant blood loss leading to the production of coagulation factors.
So, what’s the connection with COVID-19?
SARS-CoV-2, the virus causing COVID-19, is responsible for blood clot formation in 20 to 30% of critically ill patients suffering from the disease. In contrast to injury-caused clots that mainly form in limbs and bigger blood vessels, those caused by COVID-19 are more common in smaller capillaries in the lungs. Although the cause(s) of blood clot formation in COVID-19 are still not fully understood, several hypotheses have been put forward. One hypothesis is that the virus attacks endothelial cells lining the inside of blood vessels. After the virus attaches to the receptors of these cells, coagulation proteins start to produce. Another hypothesis is that the immune system in people with severe COVID-19 causes a rapid inflammation which might subsequently lead to blood clotting 3.
What about the connection with the COVID-19 vaccines?
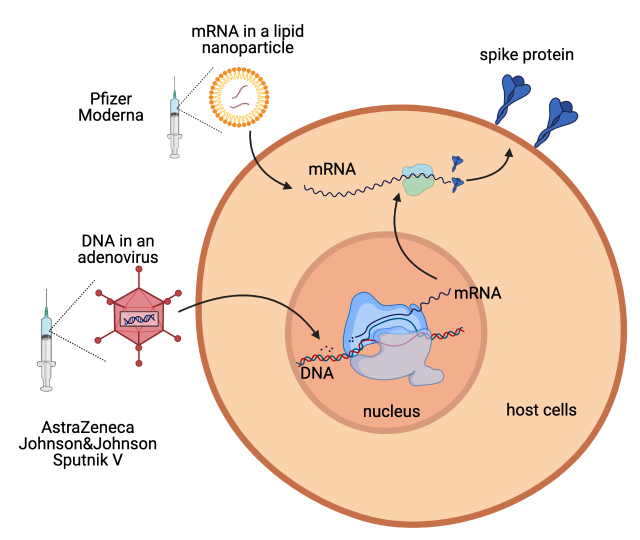
Blood clots appeared in people inoculated with the AstraZeneca and Johnson & Johnson (J&J) vaccines but not the Pfizer and Moderna vaccines. Before delving into why this might be the case, let’s first look at how these vaccines work. All four of these vaccines are based on a mechanism which, instead of a weakened virus (as seen in traditional vaccines), uses a part of the virus’ genetic information which consequently provokes an immune reaction in the body. Once we are vaccinated, the genetic information of the virus enters host cells in our body where, as mRNA (messenger ribonucleic acid), it gives instructions for protein production. The newly made viral protein is displayed on the cell surface. However, this leads to the production of just one viral protein called a “spike” protein which is unable to further reproduce in the body.
When our immune system notices a spike protein, it attempts to destroy it by generating the relevant antibodies to target it 4. These antibodies (and memory B cells which produce antibodies through forming antibody-secreting cells after the virus recognition) also protect us from further infection in the future 5. If SARS-CoV-2 enters the body, the immune system will recognise the spike proteins on its surface and release antibodies for its destruction. Thanks to these antibodies, our immune system can quickly get rid of the virus. If an individual is not vaccinated and does not have premade antibodies or long-lasting memory B cells, the destruction of the virus takes much longer. This also means that the infected person can get more ill as the body has to “waste time” producing antibodies while the virus freely multiplies, leading to a more serious reaction.
So, what is the difference between the vaccines? 6. Pfizer and Moderna are mRNA vaccines, while AstraZeneca and J&J are DNA (deoxyribonucleic acid) vaccines. While mRNA in the former vaccines is directly translated into a viral protein displayed on the surface of the cell, the DNA in the latter two vaccines has to be first transcribed into mRNA within the nucleus of a host cell. Furthermore, the vaccines differ in the composition of their shells. Pfizer and Moderna use a novel method in which the mRNA is enclosed in a lipid nanoparticle, while the DNA in AstraZeneca and J&J is encapsulated in a harmless deactivated adenovirus shell (another virus found in humans and animals causing for example a cold) 7.
Blood clots and the AstraZeneca and J&J vaccines
Apart from the above, all four vaccines are fairly similar, and yet Pfizer and Moderna do not cause blood clots, but AstraZeneca and J&J do. What’s going on with this? Interestingly, the blood clots linked to AstraZeneca are very rare and appear in unusual places, mainly in the brain and abdomen and in young people. Besides this, they consist of only a very small amount of platelets compared to normal clots, which can lead to a higher risk of bleeding. These rare symptoms are similar to the autoimmune disease heparin-induced thrombocytopenia 8, where as a result of treatment with heparin (a blood thinner), the body makes antibodies against a protein called platelet factor 4 (PF4). The PF4 protein is released from platelets after their activation and binds heparin. The binding of heparin to PF4 in this disease results in PF4 protein aggregation and the formation of relatively large clots. It also leads to the damage of platelets and the release of coagulation factors.
However, individuals vaccinated against COVID-19 are not generally exposed to heparin, so why are these side effects observed in some people? Currently, it is not known which part(s) of the vaccines are triggering this reaction. Both mRNA and DNA vaccines make spike proteins, so this protein is most likely not the cause. The most reasonable explanation is that the composition of the vaccine, and specifically the adenovirus package, causes these complications. Interestingly, apart from AstraZeneca and J&J, Sputnik V is another vaccine relying on the DNA mechanism and an adenovirus package (though we have limited data to date about whether this also leads to blood clots) 9.
Should we be concerned?
It is important to mention the rarity of blood clots after vaccination with DNA COVID-19 vaccines. To date (21st April 2021), 22 million people have been vaccinated with AstraZeneca in the United Kingdom, from whom 209 people (120 women and 89 men from 18-93 years) have developed these rare symptoms, which have unfortunately been deadly for 41 individuals. On average that is 9.3 cases per million vaccinated individuals. In other words, 0.00093%, which is incredibly rare.
When compared to the number of blood clots caused by COVID-19 itself, these vaccines are very effective and reduce coagulation risk, meaning that one is more likely to get blood clots from COVID-19 than from the vaccine itself (the exact numbers are difficult to calculate as it is not clear how many people have had the virus). Before the COVID-19 pandemic, 60,000 people were diagnosed with blood clots annually, of whom about 25% died, making blood clotting one of the leading causes of death in the UK. It follows that one is approximately 100 times more likely to get blood clots for reasons unrelated to COVID-19 vaccines than from them. Besides, those more at risk of developing blood clots, including young people, can get an alternative to the AstraZeneca vaccine 10.
In conclusion, there is no justified cause for concern as even without this extra precaution, there is a higher chance of being struck by a lightning bolt than getting blood clots after COVID-19 vaccinations.
This article was specialist edited by Georgia Beckett-Hill and copy-edited by Dzachary Zainudden.
References
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4260295/
- https://www.msdmanuals.com/home/blood-disorders/blood-clotting-process/how-blood-clots
- https://www.medicalnewstoday.com/articles/coronavirus-and-bloodclots#what-is-a-blood-clot
- Immune response after the jab and the side effects can be found here: https://healthblog.uofmhealth.org/wellness-prevention/what-happens-after-you-get-COVID-19-vaccine
- https://immunology.sciencemag.org/content/6/58/eabi6950
- Four types of vaccines and the difference between them including a short animation: https://www.gavi.org/vaccineswork/there-are-four-types-COVID-19-vaccines-heres-how-they-work
- https://www.ft.com/content/42f57da1-577c-4685-952f-2630fb0fb01a
- https://www.nejm.org/doi/full/10.1056/NEJMoa2104840
- Comparison of the efficacy of various COVID-19 vaccines: https://www.biospace.com/article/comparing-COVID-19-vaccines-pfizer-biontech-moderna-astrazeneca-oxford-j-and-j-russia-s-sputnik-v/
- Which vaccine will you get? https://www.gov.uk/government/publications/covid-19-vaccination-and-blood-clotting/covid-19-vaccination-and-blood-clotting