Brain Bibbers – The science behind anxiety

A portion of every-day life comes with worries of climate change, complemented by job insecurity and economic recessions. Not to mention the social media pressure and living in a highly competitive society, topped off with a global pandemic. Our current environment sounds like a recipe for disaster which has caused our anxiety levels to rise higher than ever. In this article, we will look into changes in our brain and neurological mechanisms that cause anxiety and quite literally make our brain bibber.
Anxiety is a natural stress response we feel in reaction to potential threats which can be physical, like an assault, or emotional, like over-bearing stress. For some, this is a transient emotion that only surfaces when a fight-or-flight reaction is required, but for others it can be a constant companion that significantly affects their everyday life. In these cases, we start speaking of anxiety disorders that come in various forms. For those with general anxiety disorder, a general state of worry and alertness triggers anxiety, whereas someone suffering from social anxiety or panic disorder will react to a specific situation. In 2013, 8.2 million people in the UK lived with diagnosed anxiety, a number suspected to increase more and more in our current climate1.
Behind the curtain of what may seem like an insignificant worry to most of us actually conceals a very complex mechanism in the brain of someone suffering from anxiety disorders. Our brain can be broadly divided into cognitive and emotional centres. We use our cognitive brain for conscious actions such as talking, planning, and problem-solving whereas the emotional brain is responsible for processing our emotions. The parts of our cerebral emotional centre driving a stress response are the amygdala, a small structure shaped like an almond in the middle of the brain, and the prefrontal cortex, a large section in the front. The amygdala functions as a danger sensor (similar to a smoke detector) and sends signals to our prefrontal cortex. The amygdala cannot differentiate between life-threatening and trivial situations and always assumes the worst-case-scenario, so the prefrontal cortex, usually in charge of controlling our emotional responses, has to keep it in check and dampen the reaction if needed. It functions as a buffer and ensures that our stress-levels are not constantly excessive. Damage in this particular area of the brain predisposes to anxiety because danger signals released by the amygdala cannot be mediated by the prefrontal cortex2.
.
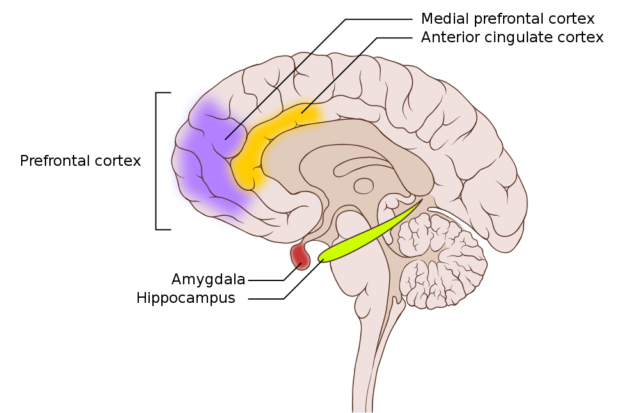
Image credit: Patrick J. Lynch, Medical Illustrator; C. Carl Jaffe, MD, Cardiologist via. Wikimedia
When looking closer at the physical symptoms of anxiety, it is fascinating how something as small as a little worry can have major effects on our body. Anxiety increases our heart rate, causes sweating, trembling, breathing difficulties, headaches, general fatigue, and muscle stiffness and impairs our ability to concentrate. Sometimes it can even mess with our digestive system and reduce our sex drive and appetite3.
Responsible for these symptoms is the interaction of the amygdala with the hypothalamic-pituitary-adrenal axis (or minus the tongue twist HPA axis) which connects the brain with the rest of our body. This axis is a one-way street for the amygdala to prompt physiological changes we need to prepare our body to flee or defend ourselves. The danger signal from the amygdala is passed on to the hypothalamus located towards the bottom of our brain where it ends in a foot-like structure called the pituitary. The pituitary is connected to a gland (the pituitary gland) and tells it to release messenger molecules that stimulate the adrenal glands. They are two of our main messenger molecule (also called hormones) factories and respond with high levels of cortisol and adrenaline production. These hormones can alter many body functions including the activity of our cardiovascular system, thus explaining the increase in heart rate, sweating, trembling and feeling of restlessness. Anxiety disorders induce this process perpetually and turn it from a life-saving instinct into a constant burden. Although very small, our amygdala is also capable of storing memory, explaining why anxiety can be associated with specific scenarios such as phobias and social situations while experiencing social anxiety.
Overcoming anxiety disorders often requires therapy and or medication4. Cognitive behavioural therapy allows retraining of the brain to dampen the fight-or-flight response and paves the way for our prefrontal lobe and cognitive brain to deal with the intense load of stress sent from the amygdala. It essentially teaches behaviourisms and coping mechanisms to our cognitive brain to stop our emotional brain from taking over with anxiety and stress. Most drugs that treat anxiety interfere with our brain chemistry, meaning they interact with molecules called neurotransmitters that the different cerebral parts use to talk to each other. Cells called neurons make up a significant part of our brain and constantly fire these neurotransmitters at each other to pass on information like a more complex version of Morse code. Depending on the type and dosage of the neurotransmitter, the messages differ and trigger different responses. Two neurotransmitters thought to be involved with anxiety disorders are glutamate and GABA which have opposing tasks5. Glutamate excites our emotional centre whereas GABA has a counteractive inhibitory function. An imbalance with more glutamate and less GABA gives stress responses more fuel and simultaneously takes off the breaks, dramatically amplifying anxiousness. A very effective medication called “benzos” are drugs that enhance the release of GABA and therefore are “putting the brakes back on”. Fortunately in some situations but unfortunately in others, our brain “has got brains” and is very good at adapting to new environments. This causes a big problem in benzo treatment as many people stop responding to the drug at some point. Antidepressants are a frequently-used alternative to benzos and function by enhancing the levels of happiness hormones in our brains to combat anxiety. They may be slightly less effective initially but do not lose their function over time. Doctors can also prescribe medication to reduce symptoms such as increased heart rate and nausea to make anxiety attacks more bearable.
Neuroscientists and psychologists spend a lot of their time exploring the nitty-gritty of very complex interactions that happen in our brain during anxiety attacks, trying to improve treatment options whether by therapy or medication. Mental health awareness has reached a new high in recent years and nearly everyone is familiar with the term anxiety these days, yet only a few understand the actual extent of the impact it can have on our lives. Anxiety is a silent illness but hopefully, together with the progress in medical research, we will pave a way for all of us as a society to deal with whatever flavoured menu every-day life has in stock for us.
This article was specialist edited by Alison Hughes and copy edited by Dzachary Zainudden.
References
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3778981/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5003319/
- https://www.nimh.nih.gov/health/topics/anxiety-disorders/index.shtml
- https://www.health.harvard.edu/a_to_z/generalized-anxiety-disorder-a-to-z
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3684250/pdf/nihms471273.pdf










