Gene Editing in HIV Therapy
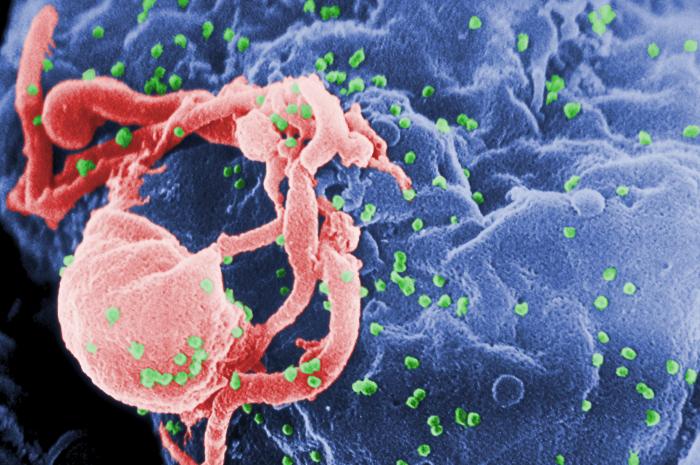
The human immunodeficiency virus, commonly known as HIV, causes the acquired immunodeficiency syndrome (AIDS). HIV infects and kills millions of people each year. In 2012, an estimated number of 35.3 million people lived with HIV 1. HIV infects mainly CD4+ T Cells, which play an important role in the body’s adaptive immune response 2. The consequently decreased number of CD4+ T Cells leads to progressive immunodeficiency and opportunistic infections, which can be life threatening. There is so far no cure for HIV.
Our immune system fights most infections by developing antibodies that bind and neutralize the pathogen. In the case of HIV it is difficult for our body to design antibodies that recognize the virus. There are several reasons why our body struggles with this task. One reason is that the virus has a very low antigen density on its surface, (also known as the ‘envelope’), which makes it difficult for bivalent antibodies to bind two antigens at the same time. Another reason for this is that the virus has a very high mutation rate. The CD4 binding site is one of the few conserved regions (which means they are resistant to mutation), but it is like other protein epitopes covered by glycans 3. So far, the virus’s ability to escape the immune system has made it impossible for successful vaccination against HIV. Therefore we need a different approach to treat this disease.
HIV binds and recognizes the T Cells CCR5 receptor. CCR5 is a chemokine (signaling protein) receptor which is suspected to be important for inflammatory responses to infection. HIV uses CCR5 as a coreceptor to enter target cells 4. Individuals that carry one mutated copy of the CCR5 gene have a much milder disease progression than individuals carrying two intact copies. Individuals with two mutated copies are resistant to HIV infection. This fact led Dr. Carl H. June and colleagues at the Abramson Cancer Family Research Institute in Philadelphia to the investigation of CCR5 mutated T Cells in mice. They mutated the CCR5 gene using zinc-finger nucleases (ZFNs). ZFNs recognize and cut specific DNA sequences, enabling mutation or deletion of certain regions. They injected ZFN mutated CD4+ cells into HIV infected mice, resulting in a much lower viral load in those mice 5. Dr June’s method has now been tested in a clinical trial with humans. Patients with chronic HIV infection received CCR5 mutated CD4+ T cells and antiviral treatment. One week later they had increased CD4+ T Cell count and blood levels of HIV DNA decreased in most patients 6. The positive effect is probably due to a positive selection for CCR5 modified T Cells as they escape HIV attacks and therefore persist longer than non-modified T Cells. The smaller number of non-modified T Cells in the circulation limits the virus reproduction capability.
The results of the clinical trial showed that the approach of gene editing to introduce a disease resistant allele is very promising. The patients’ T Cells are obtained by drawing blood and reintroduced after editing by transfusion. Both procedures described are non-invasive. It is believed that due to the selective advantage of CCR5 modified T-Cells, patients would only require consecutive treatments by gene editing after extended periods of time. Follow-up studies will show if this approach really has a long term positive outcome for HIV patients.
Edited by Debbie Nicol
References
- Read report here.
- Chan D, Kim P. HIV entry and its inhibition. Cell 1998
- Anthony P. West, Jr. et al. Structural Insights on the Role of Antibodies in HIV-1 Vaccine and Therapy. Cell 2014
- Samson M. et al. Molecular Cloning and Functional Expression of a New Human CC-Receptor Gene. Biochemistry 1996
- Perez EE, Wang J, Miller JC, et al. Establishment of HIV-1 resistance in CD4+ T cells by genome editing using zinc-finger nucleases. Nat Biotechnol 2008
- Tebas, P. et al. Gene Editing of CCR5 in Autologous CD4 T Cells of Persons Infected with HIV. New Engl. J. Med. 2014











Tebas says that the team’s ultimate goal is to wean some people off antiretroviral drugs all together. He and June are particularly excited about one study participant in whom the virus did not return during the 12-week portion of the study in which antiretroviral therapy was paused. When they examined his genome, they found that he already had one mutated copy of