Why YOU need to know about periods
With the announcement that Scotland is introducing free sanitary products for anyone who needs them1, menstrual health is making news headlines once again, but what actually is a period? And why do we need to talk about it? Let’s start with the biology behind the menstrual cycle.
The female reproductive system
Unsurprisingly, the female reproductive system is a complex one, and not only because of its anatomy. Before discussing the menstrual cycle, it’s vital to understand the key functions of each reproductive organ in turn. The female reproductive system consists of two ovaries that store, develop, and release eggs. Females possess two fallopian tubes that stretch from the ovaries all the way down to the uterus. Each month, an egg is released from one ovary into the fallopian tube. Did you know females are born with all the eggs they’ll ever have in their lifetime? This is estimated at 2 million!
The uterus, also known as the womb, provides a home and space for the development of a baby. The lining of the womb, termed the endometrium, grows into a thick tissue layer during pregnancy to support the unborn baby (foetus). Next, we have the cervix, which is found at the opening to the womb and is more commonly known as the ‘birth canal’. In non-pregnant women, the position of the cervix changes in response to each phase of the menstrual cycle.2
This is also the case in pregnant women, where the cervix dilates by up to 10 cm, allowing the baby to pass through to the vagina, and into the outside world.3‘4
The menstrual cycle and periods
Now that we have reminded ourselves of the inner structures that make up a female reproductive system, let’s talk about the menstrual cycle. The menstrual cycle is a natural sequence of changes that occur in the female reproductive system each month in preparation for a potential pregnancy. On average, a cycle lasts about 28 days but this can vary from person to person—and for a number of reasons such as underlying medical conditions and/or day-to-day stress.
The changes that occur during the menstrual cycle are tightly regulated by hormones. Hormones are chemical messengers produced by specialised cells found within organs called glands. Each hormone coordinates and regulates several biological processes, from our metabolism to the level of sugar in our blood. To understand the menstrual cycle, we will focus on four key reproductive hormones: oestrogen, progesterone, follicle-stimulating hormone (FSH), and luteinising hormone (LH). Throughout the menstrual cycle, the levels of these hormones fluctuate, giving rise to four biological phases of menstruation. More information on hormones can be found here.5
Now, let‘s talk menstruation
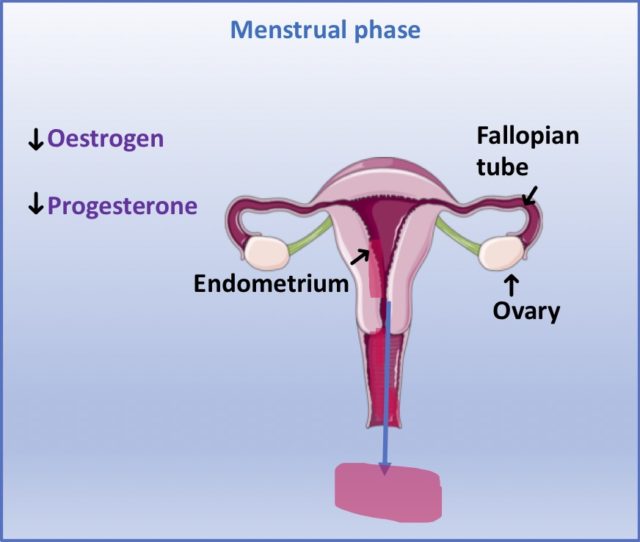
The first phase of the menstrual cycle, believe it or not, is the menstrual phase! During the menstrual phase, the endometrium is shed which results in vaginal bleeding; more commonly known as a period. This phase also coincides with a drop in production of oestrogen and progesterone by the ovaries. During the previous stage of the cycle, high levels of oestrogen had maintained a thickened endometrium, to prepare the body for embedding of a fertilised egg (implantation). Therefore, when fertilisation (fusion of the female egg and male sperm cell) is unsuccessful, implantation does not occur and a period happens!
Most females experience their first period between the ages of 10 and 16 years old, with most beginning at age 12. It is common for periods to be slightly irregular (not within the range of 21-40 days) initially, becoming more regular after a few years.6
A period can last anywhere between 3 and 7 days, with 5 days being the average. People who are on their period (as if this wasn’t enough) can also experience cramps, fatigue, back pain, mood changes, and headaches.7 Nasty, eh?
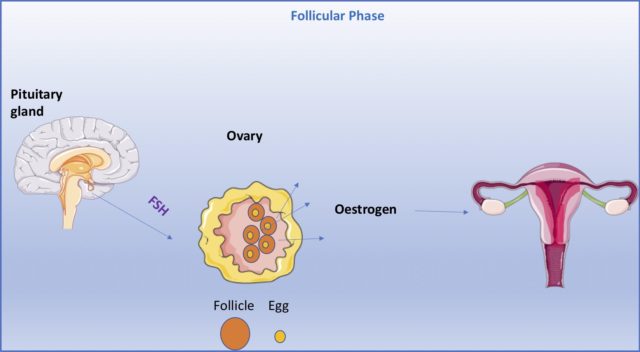
The second stage of the menstrual cycle is called the follicular phase. This phase is the most variable of the cycle and can last anywhere between 1 and 3 weeks. The follicular phase actually occurs alongside the menstrual phase and is initiated by a rise in a hormone called FSH. FSH is released by the pituitary gland in the brain and signals to the ovaries to prepare for ovulation (the release of a non-fertilised egg). This process involves the production of small sacs called follicles which contain immature eggs.8
These follicles release oestrogen, which triggers thickening of the endometrium in preparation for implantation of a fertilised egg. Only one egg matures within these follicles and this will be the one released from the ovaries during ovulation, marking the end of the follicular phase.
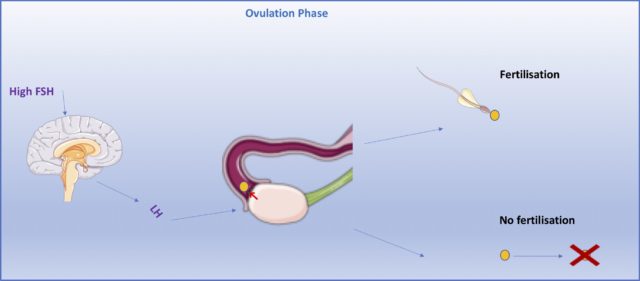
The ovulation phase follows next, whereby an unfertilised egg is released from one of the ovaries. The surge in FSH from the follicular phase triggers the pituitary gland to increase production of a hormone called LH. LH stimulates the opening of a single follicle, causing the release of an egg into the fallopian tube. Here, it begins its journey to the uterus. If the egg is fertilised, a potential pregnancy can occur. If fertilisation doesn’t happen, the egg will usually dissolve within a few days.9
Some people actually get one-sided pains in their lower abdomen during this stage, allowing them to tell when they are ovulating, and exactly which ovary has released the egg!10 Pretty cool, huh? Pretty sore, too!
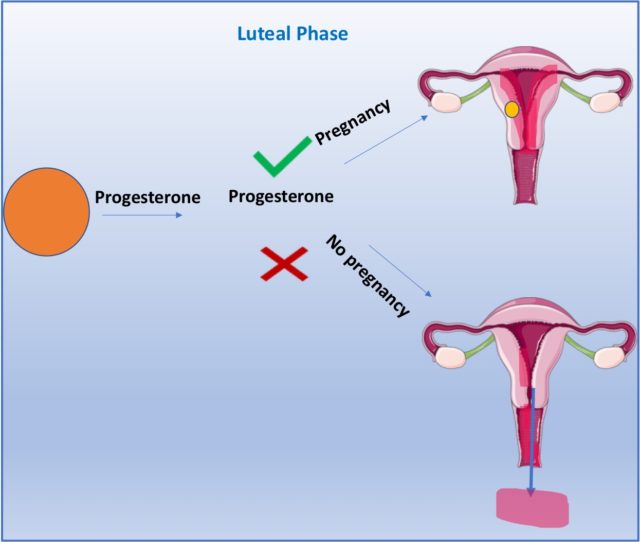
The last phase of the menstrual cycle is called the luteal phase. During this phase, the remaining follicle that contained the egg (now termed the corpus luteum) produces the hormone progesterone. If a pregnancy occurs, progesterone is produced continually to keep the lining of the womb intact for foetal development. However, if a pregnancy doesn’t occur, progesterone production of progesterone stops, the lining of the womb sheds, and the cycle starts all over again!11
So, we’ve spoken about how periods are a normal part of life for around 25% of the global population12 but now we need to talk about the taboo behind having them. Today’s society conveys periods as an embarrassment and something to be discreet about. They are most definitely not spoken about freely; the consequences of which are a lack of education about periods and, unfortunately, period poverty.
Let‘s discuss period poverty
Period poverty can be defined as the lack of access to sanitary products due to financial constraints. A recent survey revealed that as many as 1 in 10 girls had been unable to afford menstrual products.13 Period poverty is also associated with a lack of discussion about periods, which can have a huge impact on the education of people who menstruate. A survey by Plan International UK showed that around 50% of students had missed an entire day of school because of their period. Moreover, around 60% of these students felt unable to say they missed school because of their period and made up another excuse. The survey also revealed that only 1 in 5 of those who were able to go to school felt they could ask their teacher for help due to the taboo surrounding periods. Concerningly, around 70% of girls in the survey felt too embarrassed to even buy sanitary products.14 These statistics are both sad and shocking to me: first, that there is such stigma attached to a normal biological process; and second, that this stigma is having huge financial and educational effects on young people.
Of course, this isn’t a problem that’s refined to the classroom.
Periods can affect performance in the workplace too, with around 20% of people stating that the pain from their period was enough to hinder their ability to carry out daily activities. Period poverty and the embarrassment associated with periods can also lead people to take sick leave, which is often unpaid. Many people who menstruate have felt unable to talk about the issues they are facing and have even been made to feel like they are ‘overreacting’ by co-workers, creating a mental burden for them too.note]https://uk.lunette.com/blogs/news/periods-in-the-workplace [/note] The ‘Stay You Boo’ podcast does a great job of talking about the stigma associated with periods in more detail.15
How can we tackle period poverty together?
We talk about it.
Periods remain to be a hugely taboo subject—and this is a huge reason for avoidance of the problem. We need to educate all children in schools about the biology of menstruation, the social and physical difficulties associated with menstruation, and the normality of menstruation.
We need to remove the shame associated with periods.
Employers need to be educated about the challenges faced due to periods and just how detrimental it can be to ignore them. Not all periods are the same. In some individuals, underlying medical conditions such as endometriosis (where the endometrium grows in parts of the reproductive system other than the womb) can cause extreme period pain, heavy bleeding, and nausea; severely impacting a person’s ability to function in work16. Medical conditions like this may contribute to each individual’s experiences being different from that of their colleagues, and it’s important to be able to discuss this openly with employers and feel supported. Conversations about flexible working and access to sanitary products need to be initiated. Normalising this topic will only happen by talking about it.
We need to tackle the financial burden periods can have.
Scotland has been the spark for tackling this problem with the announcement that all sanitary products will be made free to those who need them. This has not only been empowering for people who menstruate but it has made periods a discussion point again, which is a massive step in the right direction to tackling the stigma attached to them. We can only hope that this will inspire other countries to follow suit.
So now that you understand how periods work and that they should not be associated with shame, you can educate others. Make menstrual health part of the conversation whenever the opportunity arises—be it at home, in pubs, during political debates, or during friendly catch-ups. Let’s do our part in the fight against period poverty and remove the stigma together.
This article was specialist edited by Holly Leslie and copy-edited by Lauren Taylor
References
- beta.parliament.scot/bills-and-laws/bills/period-products-free-provision-scotland-bill
- www.healthline.com/health/cervix-before-period
- https://www.webmd.com/sex-relationships/guide/your-guide-female-reproductive-system
- https://www.healthline.com/health/pregnancy/cervix-dilation-chart
- https://helloclue.com/articles/cycle-a-z/what-you-should-know-about-hormones
- www.nhs.uk/conditions/periods/period-problems/
- www.medicalnewstoday.com/articles/326906#the-follicular-phase
- www.healthline.com/health/womens-health/stages-of-menstrual-cycle#luteal
- www.tampax.com/en-us/period-health/menstrual-cycle-phases/
- www.nhs.uk/conditions/ovulation-pain/#:~:text=Some%20women%20get%20a%20one,middle%20of%20the%20month%22
- www.tampax.com/en-us/period-health/menstrual-cycle-phases/
- www.unicef.org/press-releases/fast-facts-nine-things-you-didnt-know-about-menstruation
- www.rcn.org.uk/clinical-topics/womens-health/promoting-menstrual-wellbeing/period-poverty#:~:text=Period%20poverty%20is%20the%20lack,regular%20occurrence%20in%20her%20life.%E2%80%9D
- www.plan-uk.org/media-centre/plan-international-uks-research-on-period-poverty-and-stigma
- https://open.spotify.com/episode/28W1zInwZ2YieXhJV1FwOb?si=gxBjlybgS5KFnbodxtVEyA&nd=1
- www.nhs.uk/conditions/endometriosis/











